
Ceramic Dental Implants Thinking about getting ceramic dental implants? You’re making the right decision! However, finding reputable dentists who can help you get ceramic implants
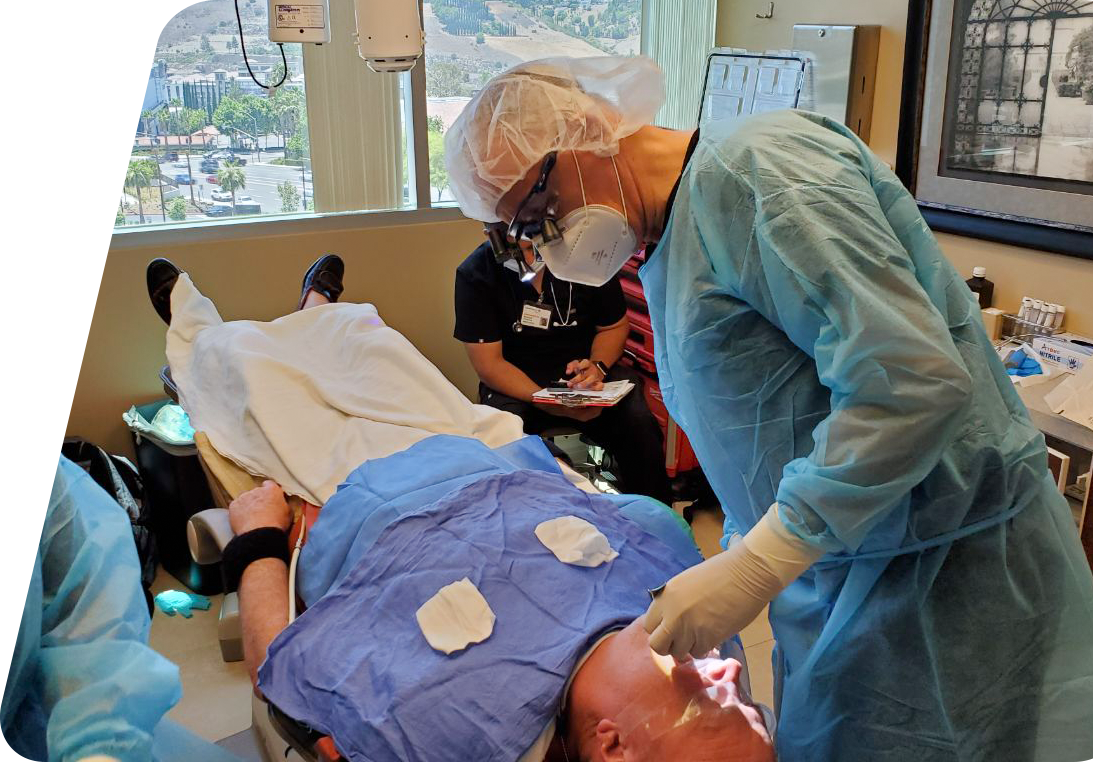


Gums can recede for several reasons, such as genes, intense brushing, and periodontal disease. Get treatment if your receding gums are exposing your roots. Due to the hypersensitivity brought on by exposed roots, they are more prone to injury and bacterial infections, which can result in gum disease and other issues. It may also hurt when you smile. The majority of patients are happily surprised by how quickly the Chao Pinhole technique helped them improve.

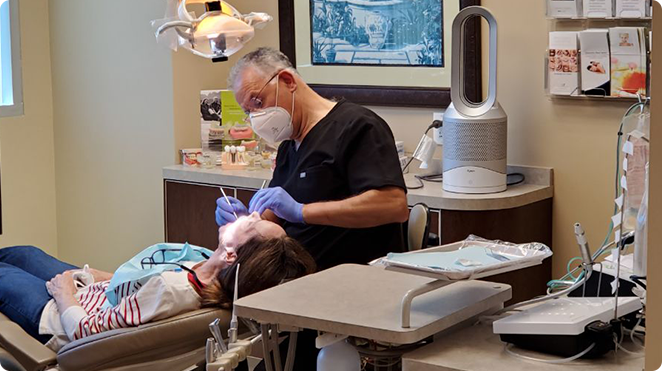
Dental implant surgery is a procedure in which the tooth roots are replaced by metal, screw-like posts, and the damaged or missing teeth are replaced with artificial teeth that closely resemble natural teeth in appearance and function.
At Mission Dental Implant Center, we want you to feel comfortable coming in for any of our dental services, and we know that sometimes that means going above and beyond what’s expected. That’s why we offer a wide range of dental services at an affordable price.
Do you and the people you care about require a dentist in Mission Viejo? Our dentists and staff are well-trained and equipped to offer compassionate, all-encompassing oral health treatment to patients of all ages. To help you obtain and keep a stunning, healthy smile, our incredible team uses the most up-to-date, exact methods and tools.
If you’re looking for exceptional dental services from family dental surgeons in Mission Viejo, get in touch with us. Our professional oral surgeons will help you find dental solutions according to your needs, whether it’s cosmetic or restorative treatment, including implants, bridges, and dentures. We’ve got an experienced team of periodontists that can provide excellent periodontal treatment to our esteemed clients in Mission Viejo.
If you’ve been thinking about getting a tooth replaced with an implant but aren’t sure how much it’ll cost or what options are available to you, our team of dentists is ready to answer your questions and help you find the best solution for your oral health requirements.

Ceramic Dental Implants Thinking about getting ceramic dental implants? You’re making the right decision! However, finding reputable dentists who can help you get ceramic implants

Laser therapy, in many cases, is an ideal alternative to surgery. In periodontal therapy and dental implant…
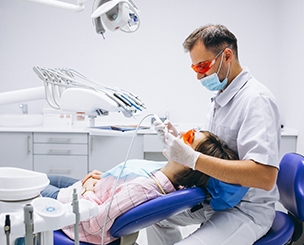
Gums can recede for several reasons, such as genes, intense brushing, and periodontal disease…..
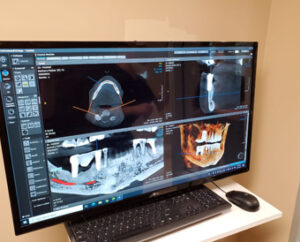
When the jawbone has been lost, a dental bone graft is required. This operation is frequently carried ….
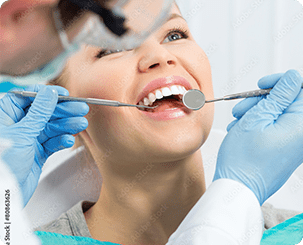
In this procedure, dental surgeons perform crown lengthening by recontouring gum tissue and sometimes bone to expose more of a tooth’s surface…..

For someone whose teeth aren’t functional, a new set of teeth could mean the world. Our daily lives are influenced by our teeth, from the food we eat to how we smile…..
The cost of a dental implant procedure is determined by the following factors:

Discovering you have one or more missing teeth can lead to considering artificial replacements and a dental bone graft is a key procedure in this

Over time, our teeth can lose their natural shine for different reasons, including getting older, eating and drinking stain-causing substances like coffee or red wine,

Laser teeth whitening, also known as laser teeth bleaching, is a cosmetic dental procedure performed in a dentist’s office. Unlike other teeth whitening methods, this

At the intersection of artistry and science, dental implant surgery emerges as a transformative procedure, replacing tooth roots with precision-engineered metal posts and seamlessly integrating
A dental implant method is when an oral physician inserts artificial enamel roots into your jawbone. These implants bond with the bone, allowing the company

Dental implants transform the world of dentistry, providing a reliable and best solution to people who suffer from tooth loss. With the increasing number of






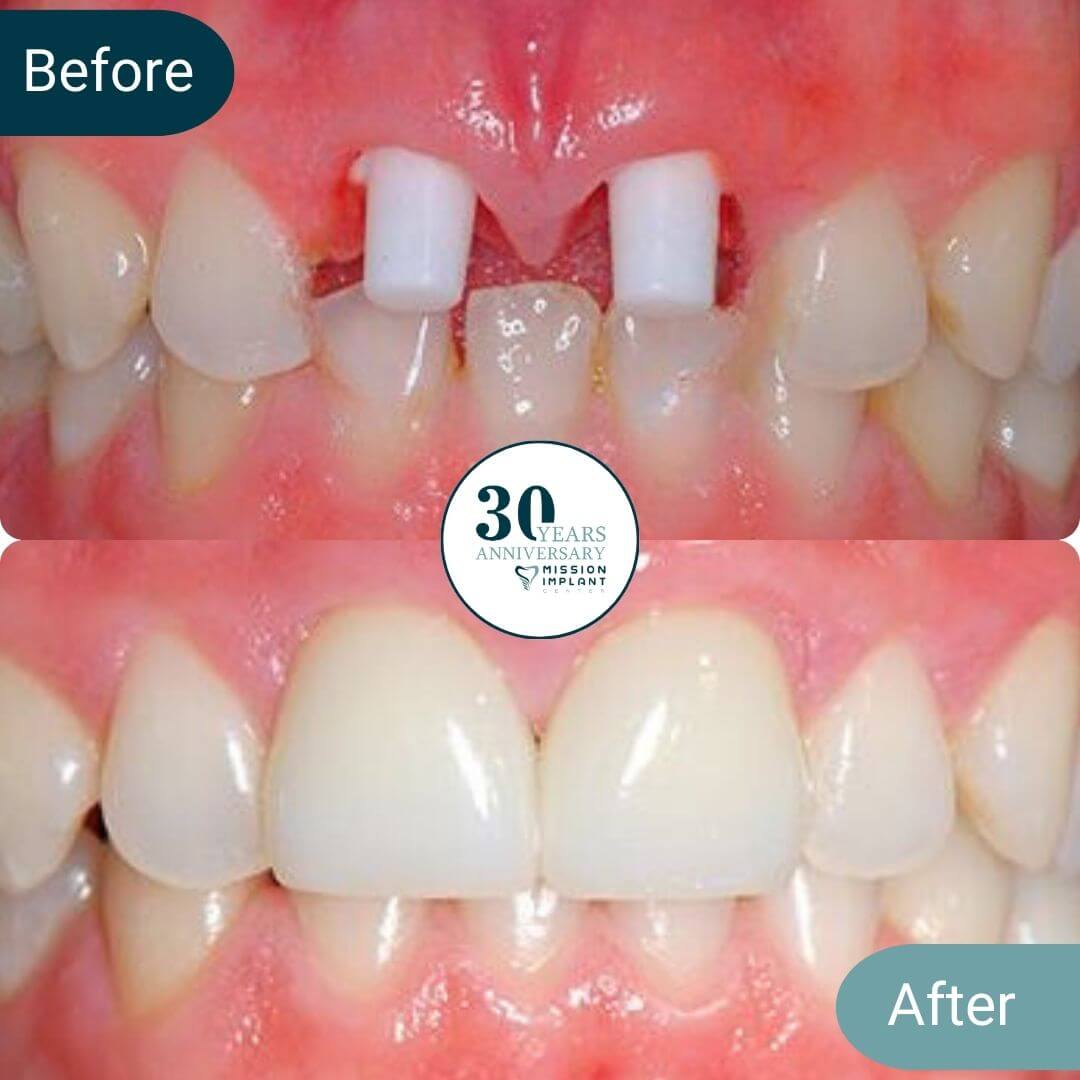
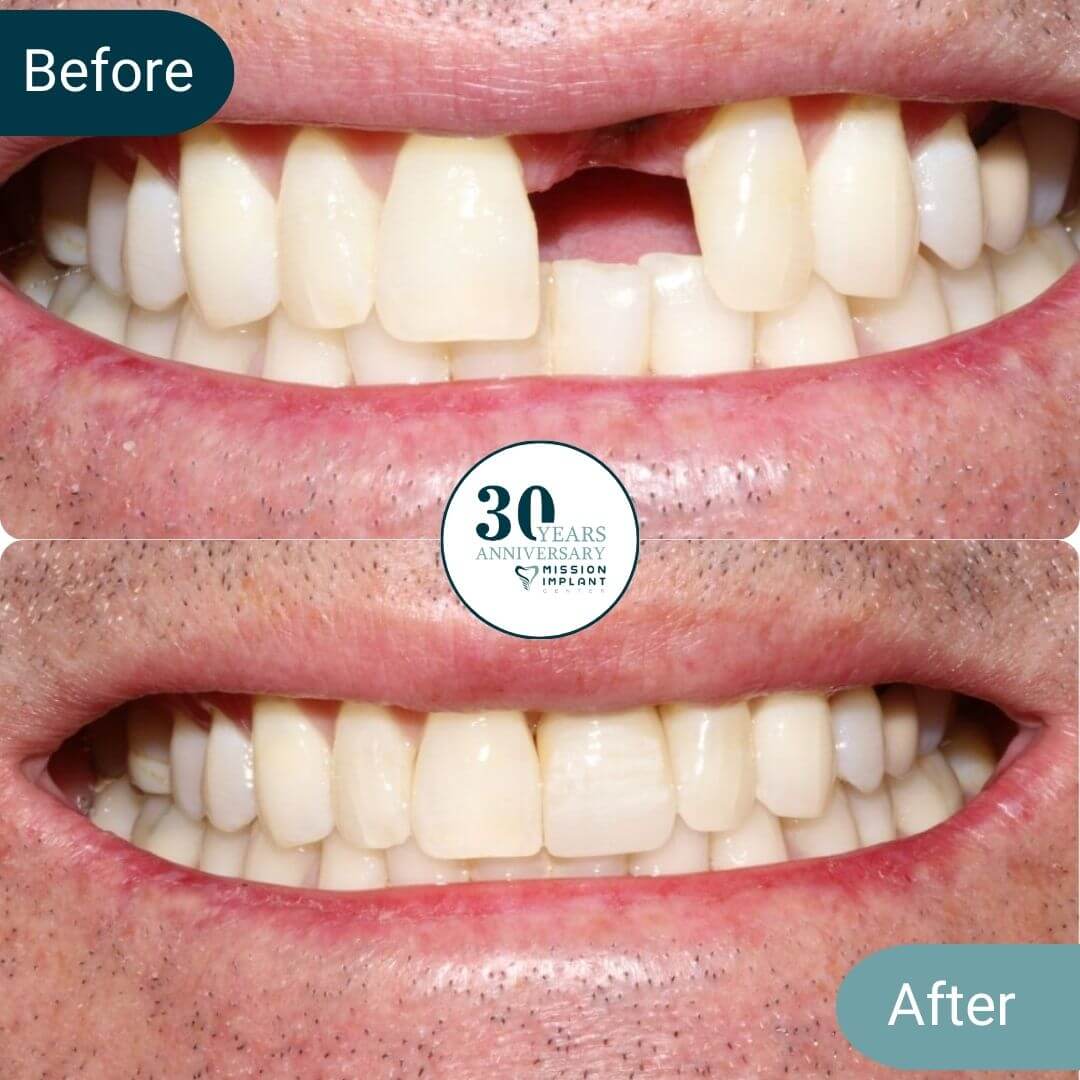
Mission Implant Center is a premier dental facility in Mission Viejo that is determined to improve your smile like never before. We want to achieve that by helping you improve your oral health so that you can look and feel great. So, book an appointment today to get started.
9:00 AM - 5:00 PM
© 2022 Mission Implant. | All Rights Reserved
Special Offer!
on your dental implant procedure! Plus, flexible financing options are available.
By signing up, you agree to receive email marketing